Coronavirus Update
I underestimated the seriousness of this pandemic when I first wrote about it just over two weeks ago in a newsletter and blog post. Two days later, I had already grown more concerned, and updated my Coronavirus blog post, but did not send out a second newsletter until now. I don’t have any good excuses for my failure to recognize the severity of this outbreak sooner, only poor ones.
Like many of you, I recalled all the panic regarding SARS in 2003, Swine flu in 2009, MERS in 2012, and others. Perhaps I felt like one of the villagers in “The Boy Who Cried Wolf” Aesop fable. Or, maybe I was just too conservative in my thinking. One of my favorite quotes from my general surgery residency is, “never be the first one on the bandwagon, or the last one off”. Generally, I think that’s pretty good advice, in life as well as in medicine, but it probably didn’t serve me well this time.

With A Little Help From My Friends
For this update, I reached out to a good friend of mine. Dustin Krutsinger is a fellow physician who is also interested in politics and policy. I met him over a decade ago, when he was still in medical school at the University of Iowa. Dustin has since completed a residency in internal medicine, a fellowship in pulmonary and critical care medicine, and a master’s degree in clinical epidemiology. He is now on staff at the University of Nebraska.
So, he’s a pretty accomplished person, and has far more expertise in this area than I do. He’s also a really good guy, and I think you’ll enjoy reading what he has to say.
Situation Update
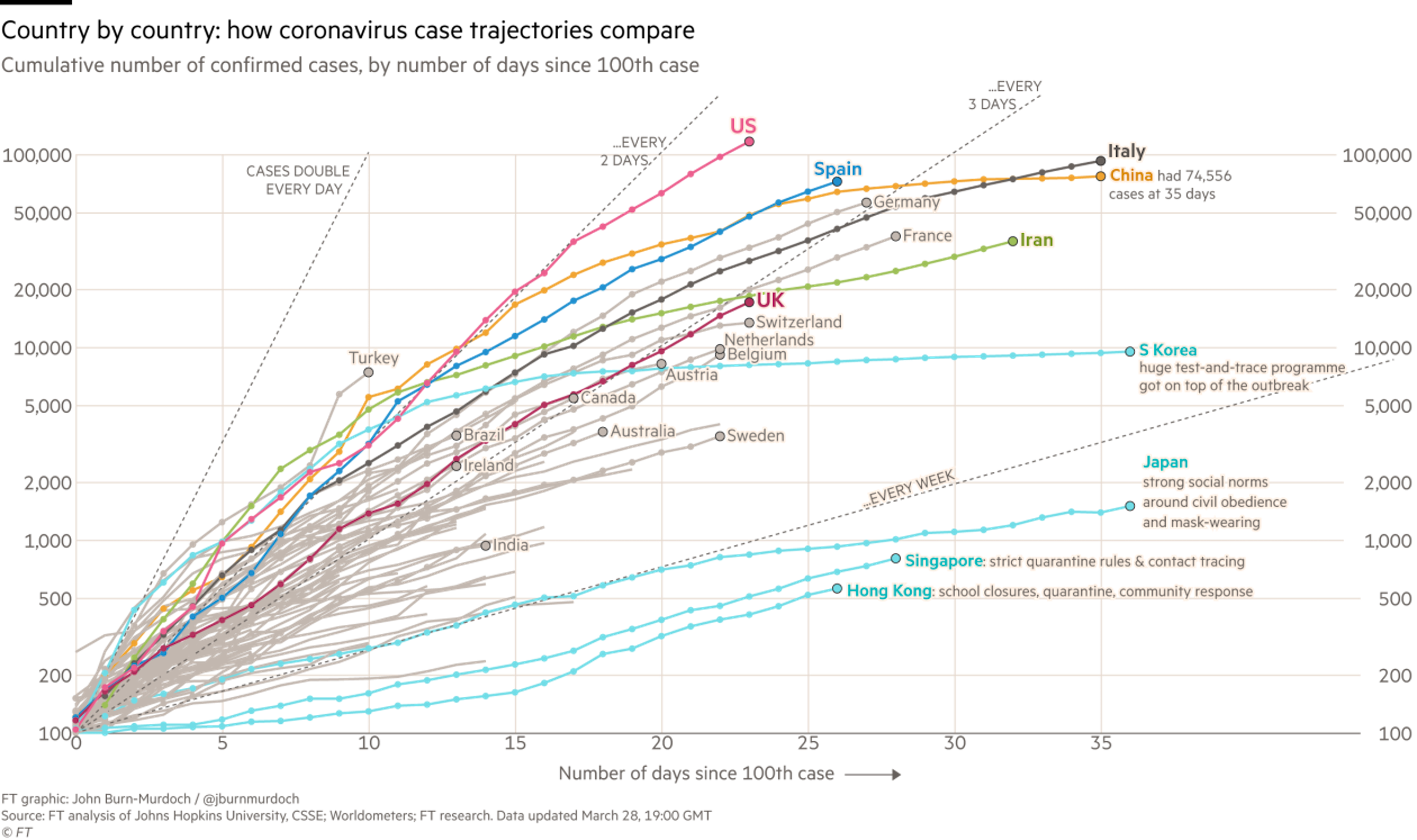
The World Health Organization (WHO) website doesn’t appear to be terribly up-to-date, especially on a per-country basis, but I’m going to use it again to make an apples-to-apples comparison. It reported 136,895 COVID-19 cases worldwide with 5,077 deaths when I first wrote about this on March 13th. As of this writing, they now report 575,444 confirmed cases worldwide with 26,654 deaths.
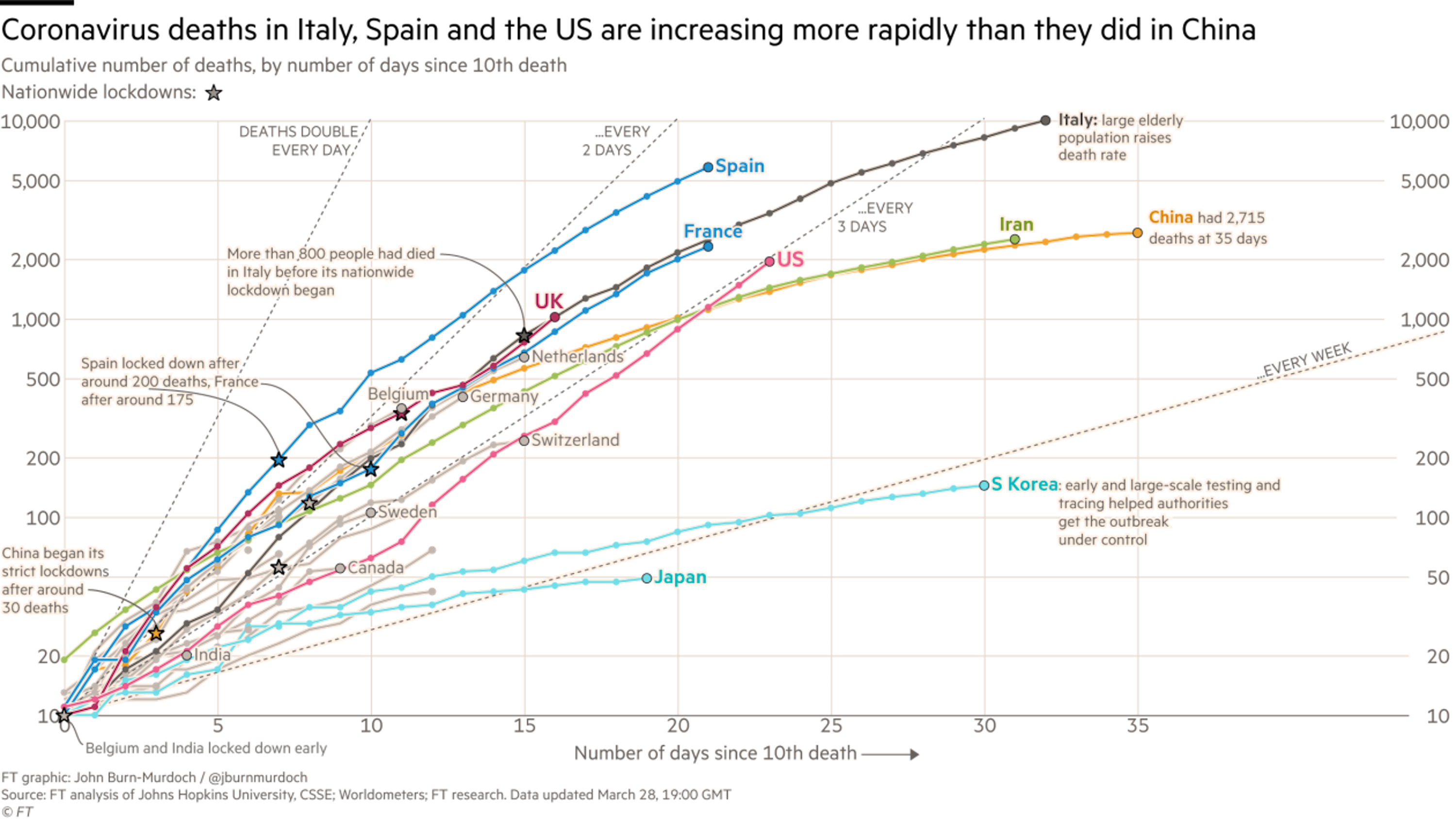
The major hotspots now appears to be Italy and Spain, which are reporting even more deaths (9,136 for Italy, 4,858 for Spain) than China (3,301). According to the Centers for Disease Control and Prevention (CDC), the United States now has 103,321 confirmed cases, more than any other country, and a total of 1,668 deaths. Domestically, New York has displaced Washington as the state with the most reported cases. It looks like there is cause for optimism in South Korea, which has had declining numbers of new cases for the last four weeks. China has also been reporting very few new cases since mid-February, but I’m skeptical of those numbers.
WHO: Coronavirus Disease (COVID-19) Pandemic
CDC: Coronavirus Disease 2019 (COVID-19): Situation Update
Dustin, any other updates you would like to add? Do you see any other sources of optimism, and should we trust China’s numbers?
The worst news certainly comes out of Northern Italy. Their system has been overwhelmed. It is not necessarily that they were hit harder than we have been here, its simply that they were hit earlier. They were hit before we realized how bad it was; before we started to think about the need to “flatten the curve”. They are a few weeks ahead of us, and we are on the same trajectory. They are being forced to make battlefield-like triage decisions in their hospitals right now.
This is why public health officials are making such a big deal out of this, why government leaders were first asking and now demanding that we take aggressive measures to slow the spread.
I’m skeptical of China’s numbers, but for better or worse we have other, more open countries, that we can learn from. The good news comes out of South Korea. They seem to have contained the virus. While there are many factors that may account for this, the general consensus is they are containing it through widespread testing and stellar epidemiological detective work, isolating those with positive test results and tracing recent contacts.
We were promised the ability to perform widespread testing two weeks ago, and we are still waiting. I personally think the ability to do widespread testing is key. We won’t be able to safely lift our social distancing measures until we have widespread testing, develop an effective vaccine or perhaps get lucky and it goes away in the summer.
Response Options
There are a number of interventions available to us. At the personal level, frequent hand washing, covering coughs and sneezes, and self-isolating when sick are obviously beneficial, have little or no apparent downside, and should be routine, pandemic or not. Public health measures, to include identifying and isolating those who are infected, and tracking down their contacts, are also definitely beneficial, as we have seen in South Korea, Singapore, and Hong Kong. Unfortunately, in many countries, to include our own, those efforts have been hampered by a much too slow rollout of screening tests, and that is still not improving quickly enough.
Beyond those measures, the public policy options include various forms of voluntary or enforced “social distancing”. They run the range from recommendations to work at home to closures of schools and businesses, from banning large (or even small) gatherings to orders to “shelter in place”. These become increasingly intrusive and have greater negative impacts at personal, societal, and economic levels.
Furthermore, it’s not at all obvious to me that we actually know which should be instituted, when and where. Even experts disagree (see below for references). Based upon the very limited evidence of which strategies are most worthwhile, I think variable responses depending upon the status of the pandemic in a given locale are perfectly reasonable. Furthermore, having different responses in different nations and states might allow us to better determine best practices for future pandemics.
NYT: The Best-Case Outcome for the Coronavirus, and the Worst
Washington Post: Facing Covid-19 Reality: A National Lockdown is No Cure
Until we have more definitive options, such as efficacious treatments for COVID-19 or an effective vaccine against SARS-CoV-2, our interventions are limited to slowing the spread of the virus (“flattening the curve”). Our near-term goal is to prevent our healthcare system from being overwhelmed, which otherwise would result in unnecessary deaths, not only from COVID-19, but also any other illnesses or injuries that might require hospitalization, and particularly a stay in the intensive care unit.
Dustin, do you think we have good evidence as to which responses are best?
In medicine, we often use the phrase, “hope for the best, but plan for the worst”. We are all hopeful that this thing blows over. That despite what we are seeing in Italy, that it just won’t be as bad here. That warm weather will arrive early and COVID-19 will act like our other seasonal respiratory illnesses and dissipate. We all hope for that. But we must prepare for the worst.
We may never know if our actions made a difference. In the coming years, epidemiologists will study these events and be able to tell us to some degree of certainty if it helped, by comparing areas that tried different strategies. But that will be in hindsight. Right now, we just don’t know for sure.
We can look to past pandemics for clues, for example the different ways Philadelphia and St. Louis handled the 1918 influenza pandemic. St. Louis was able to slow the spread dramatically by implementing social distancing measures. We can look at how other countries, who are ahead of us time-wise, are handling it and get a sense of the impact social distancing measures have had.

Primum Non Nocere
It’s important to bear in mind that many of our interventions will cause harm. School closures affect not only the education of children, but put some at risk if they are food-insecure or have an unstable home environment. School closures also cause financial stress for households, forcing parents to leave the workforce to take care of their children, as just one example.
Even in states that haven’t mandated “shelter in place”, most individuals and businesses are suffering. And, the ripple effects are tremendous. Fewer customers leads to laid off employees, fewer purchases of supplies, less advertising, outright business failures, etc. Over 3 million Americans filed first-time unemployment claims last week, easily beating the previous record of 695,000 in 1982. A global economic recession seems all but certain at this point, which will harm everyone, but especially those who are already on the lower rungs of the economic ladder. We hope this will all be short-lived, that those jobs will come back quickly once this pandemic recedes, but no one knows.
Social ties may be undermined, possibly resulting in a “social recession”, as two authors of an article in The Atlantic proposed. Will all this extra time with our spouses at home result in a “mini baby boom” in nine months, or a spike in divorces? Maybe both. Will we see a rise in violent and non-violent crime as a result of a serious economic downturn? An increase in substance abuse, depression, and suicide? Those all seem very likely to me.
NYT: Is Our Fight Against Coronavirus Worse Than the Disease?
WSJ: Record Rise in Unemployment Claims Halts Historic Run of Job Growth
The Atlantic: The Coronavirus Could Cause a Social Recession
This intersection of biology, society, and the economy is rife with peril. The COVID-19 pandemic is bad enough, but could our “cure” be worse than the disease?
Even the best treatments in medicine have side effects. Experiencing side effects doesn’t mean the treatment was ineffective or incorrect. We must be aware of the potential side effects, monitor for them, and try to treat them as the occur. In medicine, we take the best information available and try to assess the risks and benefits and see if the benefit is worth the risk.
The same is true for the measures we are taking now. There will be an impact on the economy, on households and on individuals. We have imperfect information, we don’t exactly know how bad COVID-19 will be, how effective our social distancing and other measures will be, and how bad the side effects may be. Public health officials are making judgement calls based on the best information available.
But we will not know for sure until all this is over (and even then we will likely be unable to know what the counterfactual result that might have been). So what can we do?
Listen to public health officials. Despite what your uncle may say on Facebook, he doesn’t have better information than the CDC, the WHO, or your local public health departments. There will be those who are hardest hit, experience the worst side effects.
Consider what you can do to help. Reach out to your older family, friends and neighbors. How can you help them while keeping them safe? Contact your local school to see if kids with food insecurity are being taken care of. Contact your local food bank to see if they could use some of the food that you have stockpiled. (contrary to rumor, the food supply will not shut down and you will be able to leave your home for supplies). Figure out how to maintain social ties in your community. Use technology to remain isolated but together.
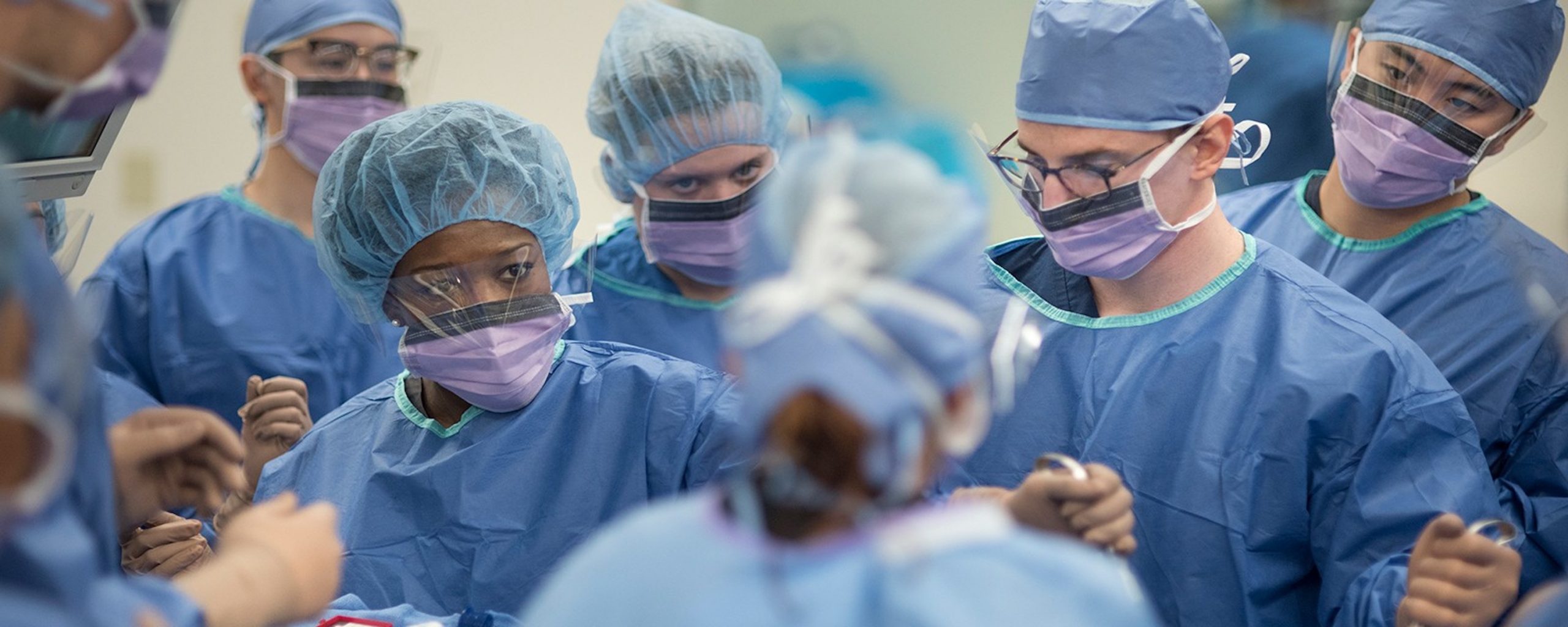
Many hospitals are already running out of personal protective equipment. If you were lucky enough to secure a box of masks, please contact your local hospital to see if they need them. They will do much more good protecting health care workers who will be continuously exposed and if infected may spread it throughout the hospital and community.
Reimagining the Future
How can we better prepare for a future pandemic (not if, but when)? How do we ensure an adequate quantity of personal protective equipment (PPE) for healthcare workers, ICU beds, and ventilators necessary? Can we find a way to better coordinate government response and information sharing within and between nations? How about coordination of research for disease treatment and prevention (vaccines)? Will we continue best practices for personal hygiene?
This is serious, but we are lucky in many ways that this is a relatively mild strain. COVID-19 is the same type of virus as SARS and MERS, both of which had a much higher fatality rate. It has exposed our system as woefully unprepared.
Hospitals are currently run as businesses. The same factors that make for a successful business make for a solvent hospital. Just in time supply delivery, having just enough hospital beds to take care of the typical demand, and hiring enough staff to do that job. That makes for a successful day to day operation, but it is insufficient for a pandemic.
There is little incentive to prepare. If hospitals had stockpiles of supplies, twice the number of beds or were paying excess staff they could not stay in business. While I’m not advocating an entire overhaul of the healthcare system, we must have an alternative way of preparing.
We assume that the government has stockpiles, but we are finding that they do not have sufficient supplies including PPE and ventilators. We must learn and be prepared for the next pandemic, which will happen.

Conclusion
Again, I apologize for underestimating this pandemic a couple of weeks ago. I also apologize for the length of this post! But, there’s obviously a lot going on with this pandemic, both as relates to the infection, itself, but also our response to it. We know far less than we would like, both in terms of this virus and the disease it causes, and the risks and benefits of our responses. We will learn more, but it’ll take time. And, we need to learn how to better prepare for the future!
Personal hygiene is important, so keep doing it! Widespread testing is needed, and our country, along with many others, has been negligent in providing it. A robust public health effort, to include identifying and isolating those infected, and tracing down their contacts, is critically important. An effective vaccination and efficacious treatments are likely still a long ways off. Until we can contain this virus through an aggressive public health effort, an effective vaccines is available, or the the virus simply dies out, social distancing remains important. There are significant downsides to this, for our economy and our humanity, and I hope we can mitigate that damage.
I’ve already provided the WHO and CDC websites, as well as several useful articles. Dustin also recommends the Johns Hopkins website. In addition, several news organizations are making their coronavirus articles free to the public.
Centers for Disease Control and Prevention
Johns Hopkins Coronavirus Resource Center
We should all do what we can. Even if it seems like very little, it all adds up! I donated a small box of surgical gowns, masks, and exam gloves to the University of Iowa Hospital two days ago. I’ve checked on some of my elderly patients to see if they need anything, but so far all are fine. I’ll continue to smile and wave at people when I go on walks or take a drive in my bus.
In my clinic, we’re still seeing a few patients, but our workload is way down. I’ve slashed our advertising budget until this is over, and cutting some personal items, too. We cancelled our cable TV service last week, switching to YouTubeTV (we like it). We’ll continue to support our local restaurants with takeout orders as our budget allows. I know most people are having to “tighten their belts” in a similar fashion.
That may be a good thing, in the long run. Maybe we’ll all learn to live a bit more prudently. Perhaps we’ll spend more time outdoors, which seems to be the case here, driven out of our homes due to boredom. I hope we’ll all learn to cherish one another a bit more after this is over, too.